When the first COVID-19 case was described in South Africa, Tygerberg Hospital (TBH) initiated an early prevention response and designed a blueprint to manage the risk of COVID-19 for pregnant women. Infrastructure was improved with additional extractor fans, oxygen and electricity points including a resuscitation and high-care area. The necessary equipment was identified, motivated for, and purchased. The hospital recruited and trained a dedicated obstetric team to work with COVID-19 positive and suspected COVID-19 obstetric patients.
The dedicated Obstetric COVID-19 Unit was established in 2020 and included an antenatal, labour, and high-care service. Up to November 2021, this dedicated COVID-19 Unit managed more than 400 women with COVID-19 or suspected COVID-19 with obstetric related emergencies or COVID-19 related emergencies.
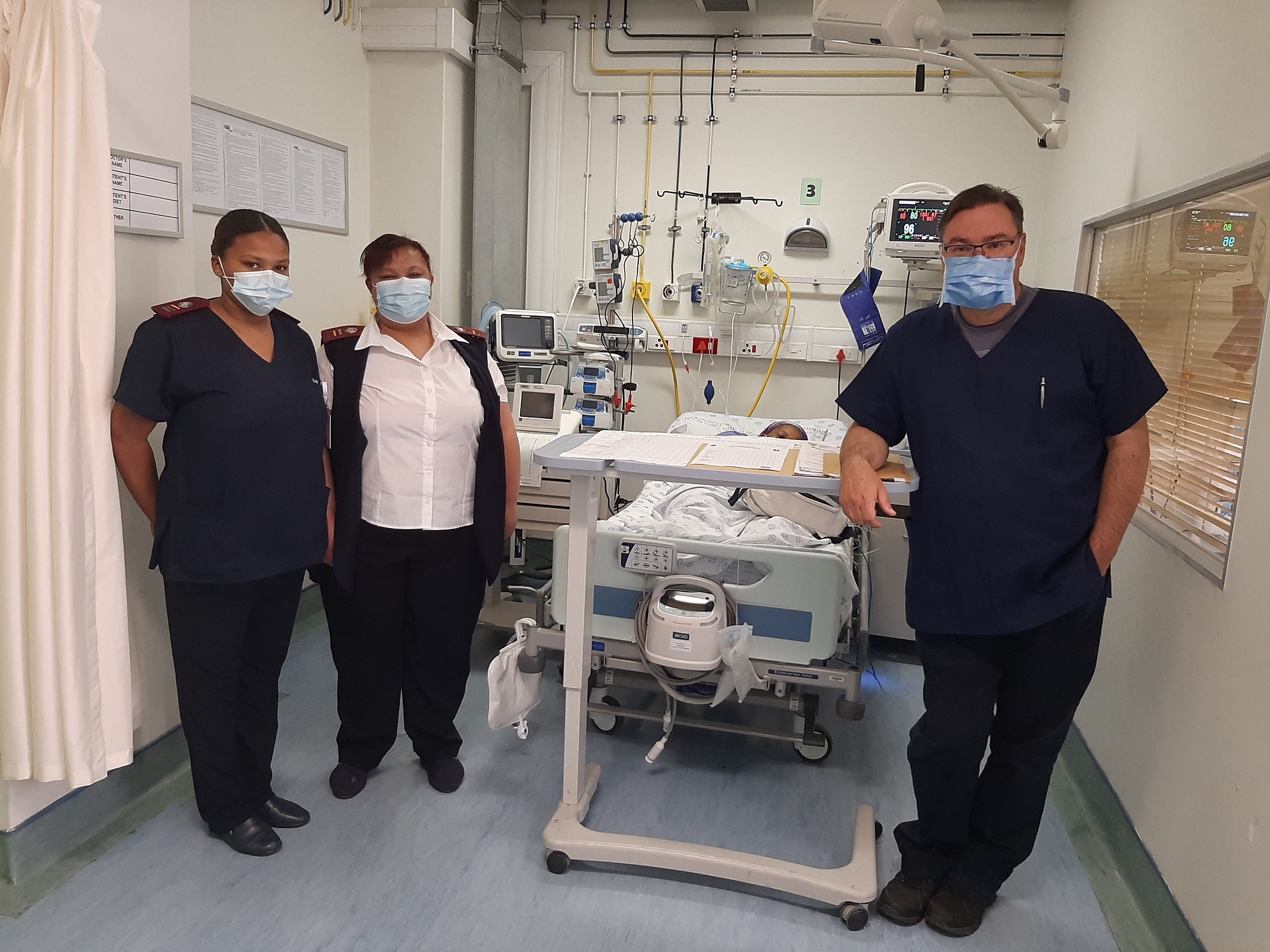
The Obstetric Critical Care Unit, where critically ill pregnant women were managed.
Pregnant women in the third trimester were more severely affected than women during early pregnancy when they developed COVID-19 pneumonia. Nearly a third of women admitted with COVID-19 required respiratory support and critical care. In more than half of the cases where women had critical disease, there was no general ICU bed immediately available. An area in the Obstetric Critical Care Unit (OCCU) was identified to manage women with life-threatening disease. The principle was to stabilise the mother and deliver the baby when indicated. These patients required High-Flow Nasal Cannula Oxygen and both non-invasive mask and often invasive ventilation. Sadly, most women who required intubation and ventilation died.
COVID-19 also affects the unborn baby. They are more likely to be born prematurely and develop other complications. When the mother becomes unstable, her unborn baby can develop hypoxia (low oxygen levels) which can result in brain damage and intra-uterine death.
Dr Eduard Langenegger, Obstetric Critical Care and Maternal Foetal Medicine specialist, said: ‘Complications, including death, is much higher in pregnant women with COVID-19. Vaccination is safe and saves mothers and babies. It is of utmost importance for eligible pregnant women to get vaccinated to protect themselves and their babies.’
There is no specific medicine that can prevent or treat COVID-19 related disease. COVID-19 vaccines are safe in pregnancy, and it is the only way to decrease risk of Intensive Care Unit (ICU) admissions and death. The availability of COVID-19 vaccines for pregnant women in South Africa was an important landmark. Despite availability, the vaccination uptake in our high-risk pregnant population was low.
To overcome this challenge, the Tygerberg Obstetric High-Risk Clinic worked together with the community vaccination centre on the premises to try to facilitate vaccination in pregnant women. They combined resources to establish a dedicated outreach vaccination area within the TBH High-Risk Antenatal Clinic. Individual risk assessment and counselling were part of the consultation.
In an audit two weeks before establishing the service on 14 September 2021, only seven pregnant women presented to the community vaccination site for vaccination. Two weeks later, 300 pregnant women were vaccinated at the Antenatal Clinic. ‘The vaccination drive resulted in more than 1 000 pregnant women attending the clinic, and may have saved many lives,’ Dr Langenegger concluded.













… [Trackback]
[…] Find More here to that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
morning jazz
morning jazz
… [Trackback]
[…] Find More to that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
stress relief
stress relief
… [Trackback]
[…] There you will find 73331 more Info on that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
… [Trackback]
[…] Information on that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
… [Trackback]
[…] Here you will find 75411 additional Info on that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
… [Trackback]
[…] There you will find 35291 additional Info to that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
… [Trackback]
[…] Read More Information here to that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
… [Trackback]
[…] Read More on on that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
… [Trackback]
[…] Read More to that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
… [Trackback]
[…] Read More on on that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
… [Trackback]
[…] Information to that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
… [Trackback]
[…] There you will find 68517 more Info on that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
… [Trackback]
[…] Information to that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
… [Trackback]
[…] Find More Information here to that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
… [Trackback]
[…] Read More Info here on that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
… [Trackback]
[…] Information on that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
… [Trackback]
[…] Info to that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
… [Trackback]
[…] Read More on to that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
… [Trackback]
[…] Info to that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]
… [Trackback]
[…] Find More here to that Topic: established.co.za/tygerberg-hospital-increases-vaccination-drive-for-pregnant-mothers/ […]